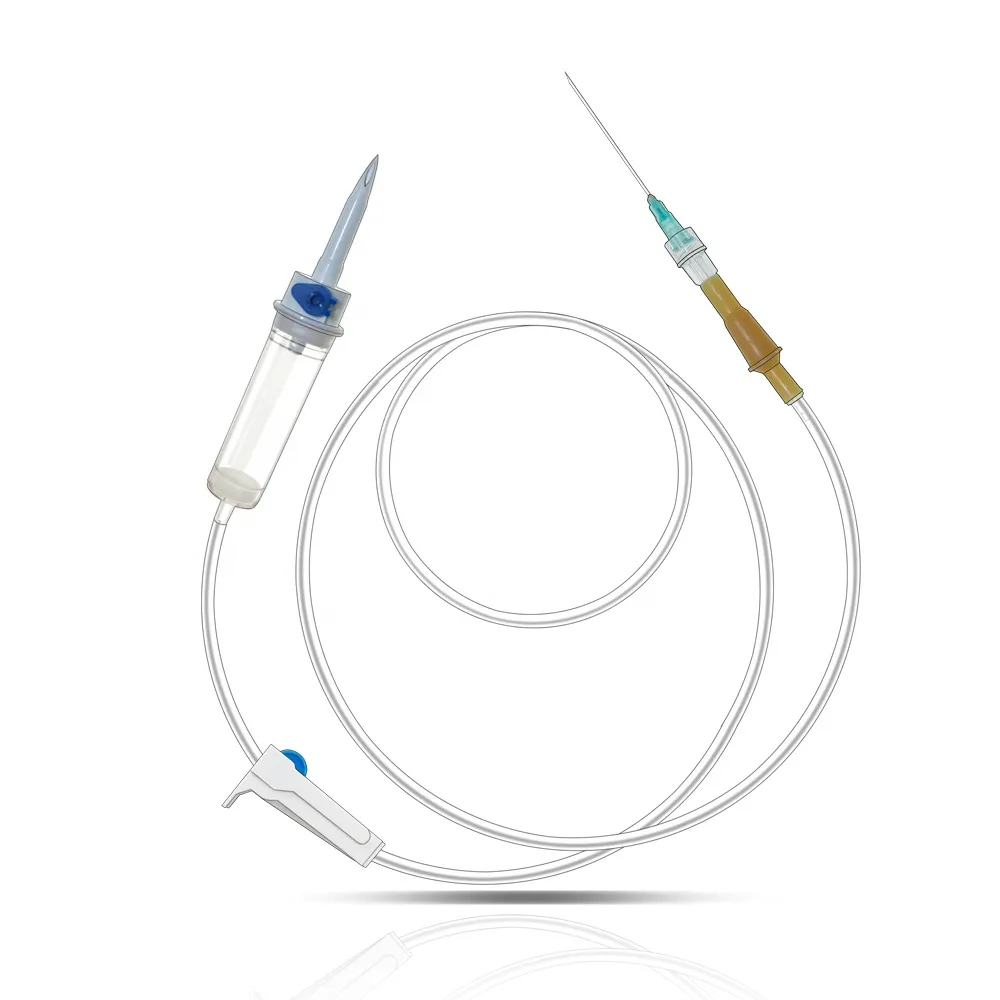
Understanding Modern Home-Based Infusion Therapy
The landscape of healthcare delivery has dramatically shifted towards home-based solutions, with infusion sets playing a pivotal role in this transformation. These essential medical devices enable patients to receive vital medications and treatments in the comfort of their own homes, reducing hospital stays and improving quality of life. As healthcare continues to evolve, infusion sets have become increasingly sophisticated, offering greater safety, convenience, and effectiveness for both patients and caregivers.
The integration of infusion sets into home healthcare represents a significant advancement in patient care, allowing for greater independence while maintaining professional medical standards. This comprehensive guide explores the various aspects of infusion sets in home settings, their benefits, proper usage, and essential considerations for optimal outcomes.
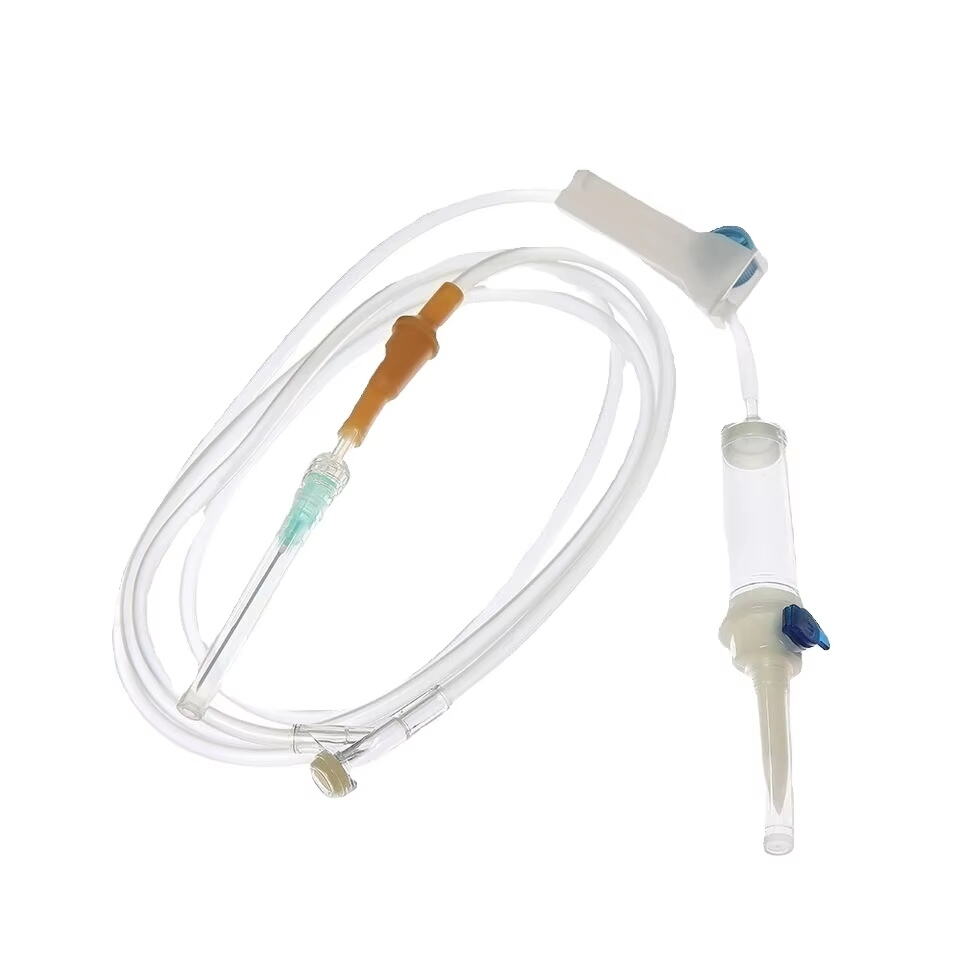
Components and Types of Home Infusion Sets
Essential Components of Modern Infusion Sets
Modern infusion sets comprise several crucial components designed for safe and effective medication delivery. The primary elements include the administration set tubing, which carries medication from the source container to the patient, and the drip chamber that helps regulate flow and prevent air bubbles. Additional components such as roller clamps, injection ports, and connectors ensure precise control and versatility in medication administration.
Advanced infusion sets also incorporate safety features like back-check valves and air-eliminating filters, providing multiple layers of protection against complications. These components work together seamlessly to deliver accurate medication doses while maintaining sterility throughout the treatment process.
Different Types for Specific Applications
Home healthcare settings utilize various types of infusion sets, each designed for specific therapeutic needs. Gravity-dependent sets rely on gravitational force for medication delivery, offering simplicity and reliability for basic infusion needs. Electronic pump-compatible sets provide precise control over medication flow rates and are essential for complex treatment protocols.
Specialty infusion sets cater to specific medical requirements, such as light-sensitive medications, pediatric applications, or blood product administration. Understanding the appropriate type for each situation ensures optimal treatment outcomes and patient safety in the home environment.
Safety and Maintenance Protocols
Proper Handling and Storage Guidelines
Maintaining the integrity of infusion sets requires strict adherence to handling and storage protocols. All components must be stored in clean, dry environments at appropriate temperatures to prevent degradation. Regular inspection of packaging integrity and expiration dates is crucial for ensuring device safety and effectiveness.
Healthcare providers must educate patients and caregivers about proper handling techniques, including hand hygiene, aseptic technique, and the importance of maintaining a clean environment. These fundamental practices help prevent contamination and ensure successful treatment outcomes.
Regular Maintenance and Replacement Schedules
Establishing and following proper maintenance schedules is essential for optimal infusion set performance. Regular assessment of all components, including tubing integrity, connection security, and filter functionality, helps identify potential issues before they affect treatment. Healthcare providers should develop clear guidelines for component replacement based on manufacturer recommendations and clinical requirements.
Documentation of maintenance activities and any observed issues helps track performance patterns and anticipate potential problems. This proactive approach to maintenance significantly reduces the risk of complications and ensures consistent medication delivery.
Patient Education and Training
Essential Skills for Home Care Success
Comprehensive patient education forms the foundation of successful home infusion therapy. Healthcare providers must ensure that patients and caregivers understand proper setup procedures, infection control practices, and troubleshooting techniques. Hands-on training sessions allow individuals to develop confidence in managing their infusion sets independently.
Education should cover recognition of common problems, appropriate response procedures, and when to seek professional assistance. This knowledge empowers patients to maintain their therapy safely while identifying potential complications early.
Monitoring and Documentation Requirements
Accurate monitoring and documentation are crucial aspects of home infusion therapy. Patients must learn to track important information such as infusion times, medication volumes, and any unusual observations during treatment. This data helps healthcare providers assess treatment effectiveness and make necessary adjustments.
Regular communication between patients and healthcare providers ensures optimal therapy management and prompt attention to any concerns. Clear documentation procedures help maintain continuity of care and support positive treatment outcomes.
Troubleshooting Common Issues
Identifying and Resolving Flow Problems
Flow-related issues are among the most common challenges in home infusion therapy. Understanding how to identify and address problems such as slow flow rates, occlusions, or air in the line helps maintain treatment continuity. Simple troubleshooting steps, when properly executed, can often resolve these issues without requiring professional intervention.
Patients should be familiar with basic troubleshooting procedures while recognizing situations that require immediate professional attention. This balanced approach ensures safety while promoting independence in managing routine challenges.
Managing Equipment Malfunctions
Equipment malfunctions can occur despite proper maintenance, making it essential for users to understand appropriate response procedures. Clear guidelines for identifying equipment issues, implementing temporary solutions, and accessing support services help minimize treatment interruptions.
Having backup supplies and equipment readily available ensures continuous therapy even when problems arise. This preparedness, combined with knowledge of proper response procedures, helps maintain treatment effectiveness and patient safety.
Frequently Asked Questions
How often should infusion sets be replaced in home care settings?
Infusion sets typically require replacement every 24-96 hours, depending on the type of therapy and manufacturer guidelines. Specific medications may require more frequent changes, and sets should always be replaced immediately if contamination is suspected or integrity is compromised.
What are the signs of infusion set complications that require immediate attention?
Key warning signs include unusual pain or swelling at the insertion site, redness or warmth around the catheter, fever or chills, and visible damage to any component of the infusion set. These symptoms require immediate professional evaluation to prevent serious complications.
Can infusion sets be reused or cleaned for multiple uses?
Infusion sets are designed for single use only and should never be reused or cleaned for multiple applications. Reusing sets increases infection risk and may compromise medication delivery accuracy. Always use new, sterile components for each setup.
What special considerations apply when traveling with infusion sets?
When traveling, maintain proper temperature control for supplies, carry necessary documentation and emergency contacts, and pack extra supplies. Consult healthcare providers about specific travel requirements and potential adjustments to maintenance schedules based on different time zones or environmental conditions.